ИЗМЕНЕНИЕ ПРОФИЛЯ ЦИТОКИНОВ ПРИ ПРОГРЕССИРОВАНИИ ХРОНИЧЕСКОЙ ОБСТРУКТИВНОЙ БОЛЕЗНИ ЛЕГКИХ
Виткина Т. И.1, Денисенко Ю. К.1, Давыдова К. А.2
1Доктор биологических наук, Владивостокский филиал ФГБУН «Дальневосточный научный центр физиологии и патологии дыхания» - НИИ медицинской климатологии и восстановительного лечения, 2Магистрант, Дальневосточный федеральный университет
ИЗМЕНЕНИЕ ПРОФИЛЯ ЦИТОКИНОВ ПРИ ПРОГРЕССИРОВАНИИ ХРОНИЧЕСКОЙ ОБСТРУКТИВНОЙ БОЛЕЗНИ ЛЕГКИХ
Аннотация
Цель данного исследования – описание изменений цитокинового профиля пациентов по мере прогрессирования хронической обструктивной болезни легких (ХОБЛ). В работе был определен и проанализирован профиль циркулирующих цитокинов (IL-4, IL-6, IL-10, IL-17А, IL-21, TNF-α, IFN-γ, TFG-β1) у пациентов с хронической обструктивной болезнью легких (ХОБЛ) разной степени тяжести в стадии ремиссии. Но основе этих данных были определены типы Т-хелперного ответа, характерные для данной патологии. Результаты исследования могут быть использованы для улучшения диагностики и лечения пациентов с ХОБЛ.
Ключевые слова: ХОБЛ, T-хелперы, цитокины.
Vitkina T. I.1, Denisenko Yu. K.1, Davydova K. A.2
1PhD in Biology, Vladivostok Branch of Far Eastern Scientific Center of Physiology and Pathology of Respiration – Research Institute of Medical Climatology and Rehabilitation Treatment, 2Master’s Degree student, Far Eastern Federal University
THE CHANGES IN THE PROFILE OF CYTOKINES IN PROGRESSING CHRONIC OBSTRUCTIVE PULMONARY DISEASE
Abstract
The aim of this study was to describe changes in cytokine profile in patients with progressing chronic obstructive pulmonary disease (COPD). The profile of circulating cytokines (IL-4, IL-6, IL-10, IL-17A, IL-21, TNF-α, IFN-γ, TFG-β1) was determined and analyzed in patients with progressing COPD of varying severity in remission. These data were used to reveal types of T-helper response, which are typical for this pathology. The results can be used to improve the diagnosis and treatment of patients with COPD. Keywords: COPD, T-helpers, cytokines.Chronic obstructive pulmonary disease (COPD) is a progressive disease characterized by airflow limitation associated with significant chronic inflammatory response of the lungs to noxious particles or gases [5]. COPD is characterized by inflammatory response of a local and a systemic nature. The systemic inflammation is primarily due to the increased concentration of blood pro-inflammatory cytokines. The balance of cytokines determines the activation of T-helper cells (Th-cells), which includes several subsets. The activation of different types of the adaptive immune response is associated with the type of Th-cells that were activated through antigen presentation [3]. The producing of a large number of IFN-γ (interferon-γ) that provides the activation of macrophages, NK-cells (natural killer cells) and cytotoxic T-lymphocytes is feature of Th1-type immune response. Th17-type immune response is mediated by the producing of IL-17 (interleukin-17) that activates neutrophils, macrophages, and epithelial cells [2]. It is believed that Th17-cells contribute to the development of chronic pathological inflammation and play a negative role in the course of the disease [3]. The purpose of this study was to describe changes in cytokine profile in patients with progressing COPD.
Materials and methods.
The study population consisted of 112 patients (age 57,5 ± 4,8 years) with stable mild (36 people), moderate (52 people) and severe (24 people) COPD in remission and 32 healthy, non-smoking individuals with normal lung function (age 42,0 ± 3,4 years) [5]. All participants have given a voluntary informed consent. Serum levels of TNF-α (tumor necrosis factors α), IL-4 (interleukin 4), IL-6, IL-10, IL-17А, IFN-γ (interferon γ) were determined by using multiplex quantitative flow cytometry (test-system Cytometric Bead Array BD, USA). Serum levels of TFG-β1 (transforming growth factor β1) and IL-21 were determined by using ELISA (enzyme-linked immunosorbent assay) (Genzyme diagnostics, USA). Data were described as median values with interquartile range. Differences between groups were evaluated by using the Mann–Whitney U-test. Differences was considered significant at p-value < 0,05.
Results and discussion.
The different types of immune response (with the participation of Th1- and Th17-cells) have been identified during the study of cytokine profile in patients with stable COPD of varying severity. The direction of the development of immune response in the study groups was evaluated by the level of circulating cytokines. For the most patients with mild COPD the disease occurred in accordance with the Th1-type immune response (67% of patients), Th17-type was identified in less number of patients (33% of patients). In the next stages of the disease the Th17-type of immune response began to prevail – for 54% of patients with moderate COPD, and 75% of patients with severe COPD.
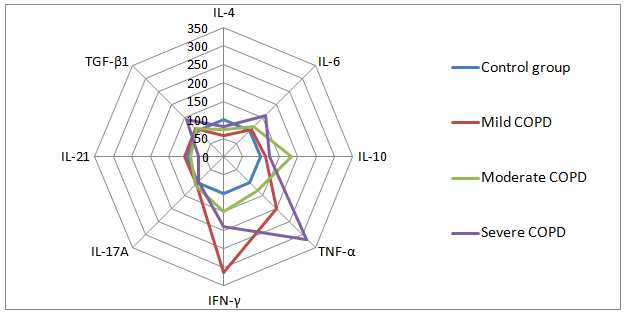
Fig. 1 - Cytokine profile in patients with COPD of varying severity with Th1-type immune response (percentage relative to the control group taken as 100%)
The findings indicated an increase in the levels of IFN-γ and TNF-α cytokines providing mobilization of inflammatory response for COPD patients with Th1-type immune response in all stages of the disease. At the same time the levels of anti-inflammatory cytokine IL-4 remained below reference value throughout all stages of the disease. The deficiency of IL-4 and high IFN-γ and TNF-α levels indicate the failure of Th1-dependent pathway of inflammation (fig. 1).
The maximum IFN-γ concentration (concentration was increased up to 3 times in comparison with the control group) and the decrease in TNF-α levels (2 times higher than in the control group) were detected in patients with mild COPD developing by the Th1-pathway. The main role of IFN-γ and TNF-α in inflammation is the activation of macrophages. IFN-γ and TNF-α levels were increased of 164% and 72%, respectively in patients with moderate COPD, but were significantly lower, than the corresponding levels in patients with mild COPD. Perhaps it is due to an increase anti-inflammatory IL-10 concentration in this stage. The serum level of TNF-α was ranked first among pro-inflammatory cytokines in patients with severe COPD (the level was increased by 3.2 times compared to the control group level) (fig. 1).
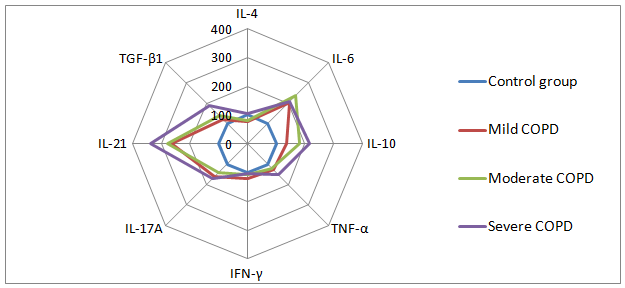
Fig. 2 - Cytokine profile in patients with COPD of varying severity with Th17-type immune response (percentage relative to the control group taken as 100%)
According to the results, the hyperproduction of IL-21, IL-6, IL-17A, TGF-β1 and IL-10 was observed in COPD patients with the Th17-type immune response in all stages. Besides that, there was an increase in the circulating TNF-α levels during progression of COPD (fig. 2). Cytokines, such as IL-21, IL-6 and TGF-β1, direct the differentiation of Th0-cells towards Th17-cells providing the prolongation of the immune response. Accordingly, the increase in the levels of these cytokines leads to the increase in the numbers of Th17 cells as the disease progresses [2, 4]. In turn, Th17-cells activate the synthesis of TNF-α, IL-6 and other pro-inflammatory factors and provide the mobilization of neutrophils and macrophages at the site of inflammation by the production of IL-17A [2]. IL-10 inhibits IFN-γ production by T-lymphocytes and pro-inflammatory cytokines production by macrophages. Probably due to this, the IFN-γ levels were increased in patients with mild COPD whereas the concentration of IL-10 was not so high. In patients with moderate and severe COPD the IFN-γ levels were within the normal range due to IL-10 accumulation in the blood (fig. 2). It has been found that the higher levels of all studied cytokines in the peripheral blood were typical for patients with severe COPD progressing towards Th17-type immune response, in comparison with patients with Th1-type of the immune response.
Conclusion.
In mild COPD in remission the development of pathology occurs predominantly by Th1-type immune response, as it was observed. As the disease progresses, the Th17-type immune response starts to prevail. In the serum of patients with COPD progressing by Th1-pathway high IFN-γ and TNF-α levels and low IL-4 levels were indicated for all stages of the disease. The maximum IFN-γ concentration along with lower TNF-α concentration was detected in patients with mild COPD and Th1-type immune response. In moderate COPD IFN-γ and TNF-α level were significantly decreased and at the same time IL-10 levels were increased. On the severe stage of COPD TNF-α becomes the most increased in levels cytokine. For COPD patients with Th1 immune response the progression of pathology was accompanied by an increase in IL-21, IL-6, IL-17A, TGF-β1, IL-10 and TNF-α levels and a decrease in IFN-γ concentration. The impact of T-lymphocytes developing towards Th1- or Th17-ways should be taken into account during the treatment of COPD. Furthermore, therapy should be personalized and based on the spectrum of cytokines produced by Th1- or Th17-cells.
References
- Ketlinskiy S. A. The role of T-helper cells types 1 and 2 in the regulation of cellular and humoral immunity // Allergy, asthma and clinical immunology. 2000. V. 8. P. 87-91.
- Kologrivova I. V. Molecular aspects of the functioning T-helper type 17 / I. V. Kologrivova, E. N. Kologrivova, Т. Е. Suslova // Bulletin of the Siberian medicine. 2011. №. 4. P. 93-99.
- Rekalova Е. М. The immunopathogenesis of chronic obstructive pulmonary disease // Ukrainian pulmonology journal. 2012. №. 2. P. 35-37.
- Rincon M. Role of IL-6 in asthma and other inflammatory pulmonary diseases / M. Rincon, C. G. Irvin // International journal of biological sciences. 2012. V. 8. №. 9. P. 1281.
- Global initiative for chronic obstructive lung disease: global strategy for the diagnosis, management, and prevention of chronic obctructiv pulmonary disease [Electronic resource]. – 2014. – Mode of access: http://www.goldcopd.org/uploads/users/ files/GOLD_Report_2014_Jun11.pdf.
